Page 6 - 21st Century Perspective - Glaucoma Supplement
P. 6
integrity, particularly the inferotemporal and superotemporal tissues of the optic nerve, as these
tissues are most susceptible to IOP microtrauma (Figure 1).
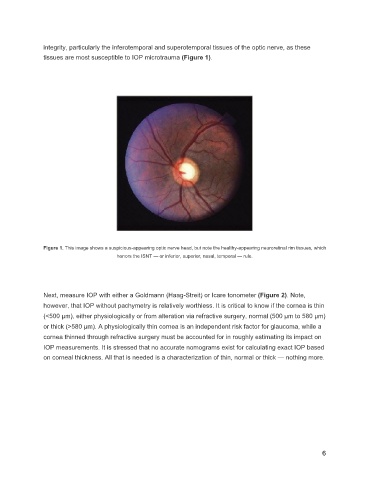
Figure 1. This image shows a suspicious-appearing optic nerve head, but note the healthy-appearing neuroretinal rim tissues, which
honors the ISNT — or inferior, superior, nasal, temporal — rule.
Next, measure IOP with either a Goldmann (Haag-Streit) or Icare tonometer (Figure 2). Note,
however, that IOP without pachymetry is relatively worthless. It is critical to know if the cornea is thin
(<500 µm), either physiologically or from alteration via refractive surgery, normal (500 µm to 580 µm)
or thick (>580 µm). A physiologically thin cornea is an independent risk factor for glaucoma, while a
cornea thinned through refractive surgery must be accounted for in roughly estimating its impact on
IOP measurements. It is stressed that no accurate nomograms exist for calculating exact IOP based
on corneal thickness. All that is needed is a characterization of thin, normal or thick — nothing more.
6